In my professional work with people who have migraine and the thousands of people I interact with on social media platforms, much of the conversation is around migraine-oriented eating. I’m a registered dietitian as well as a certified health and wellness coach focused on working with people living with migraine. There is no denying that there is a relationship between sugar and migraine attacks for a significant percentage of people.
I shuddered at the very idea of not having sugar in my life. As a matter of fact, I thought those who banished sugar from their lives were extremists. Let me assure you that I am not a zealot who is going to tell you that you need to breakup with sugar in order to get your migraine attacks in good control. Personally, sugar is not a migraine trigger for me but I feel better overall when I limit it.
Let’s take a good look at what may be going on. If you notice a relationship between sugar and migraine attacks the below information will be important to know.
** While Migraine Strong writes about the latest in migraine treatments, this is not medical advice. We are patient educators and all information you read should be discussed with your doctor.
4 possible reasons for sugar and migraine episodes
1. Fluctuating blood sugar levels = sugar migraine
When we eat food, our body gets to work on digesting and absorbing the meal. Assuming our digestive and endocrine systems are working properly, there is a normal, healthy rise in blood sugar followed by a gradual decline. Blood sugar is kept in a range that allows our body to have enough fuel to provide the brain and all organs of the body to perform vital functions.
For some people, the ability to regulate blood sugar is impaired. Blood sugar levels may climb too high in response to sugars and other high-carbohydrate foods. Their body may sense this elevated blood sugar and respond with a surge in a hormone called insulin to try to reduce the elevated blood sugar. The surge sometimes results in blood sugar getting too low. This can cause “sugar headache” for those who are prone to it.
The migraine brain is often described as being hyper responsive to normal, benign stimulation. A person who is not prone to sugar migraine attacks may be completely unaware of the ups and downs of their blood sugar whether they are normal fluctuations or not.
Contrarily, the person predisposed to migraine may be triggered by the inconsistencies and abnormalities in blood sugar. With this theory about sugar and migraine attacks, the body is sometimes unable to maintain blood sugar in the proper range. This causes the brain to respond with pain as a warning signal that something is wrong.
This response to the low blood sugar level is described as a “sugar headache”. Yet, quite a few of us often experience headaches that quickly escalate to migraine when not treated early enough.
A leading expert’s opinion on sugar and migraine
Dr. Alexander Mauskop is one of world’s authorities on headache disorders. In his recent book, The End of Migraines- 150 Ways to Stop Your Pain, he states:
Sugar is not always an obvious trigger. Many people develop migraine hours after a carbohydrate-rich food. Three-quarters of people with migraine have reactive hypoglycemia. This means that their blood sugar drops too low after a carbohydrate-rich meal.
3 steps to take to avoid sugar migraine episodes
First, know the signs of hypoglycemia aside from headache such as shakiness, sweating, confusion and hunger. You may only recognize the sugar headache, but that should be reported to your doctor. He/she will ask you more questions and determine if further testing needs to be done to figure out if your blood sugar is stable and if something else should be done.
Second, pay attention to the types of foods in your meals and snacks and make sure that if you have a sugary food, you pair it with a good protein, fat and/or fiber source. Protein, fat and fiber slow the digestion and absorption of sugar into the blood stream. So, if you have a sweet tooth and enjoy candy as an afternoon snack, consider switching to honey-roasted nuts.
Nuts are a good source of protein, fat and fiber. Or, if you must have a cookie, wash it down with a little whole milk.
In general, if you already suspect sugar and migraine attacks are linked for you, you should limit sugary foods and meals that are high in sugar and/or simple carbohydrates.
Third, do not skip meals. Not having food when your body is used to having nourishment can make your blood sugar dip and set you up for a hunger-headache or migraine. Additionally, you may tend to overeat and indulge in too much sugar/carbs when you have your next meal. Your blood sugar could be spiking and falling throughout the day and antagonizing your hyper-responsive brain.
If you have headaches that come and go, consider blood sugar fluctuations as one possible cause.
The migraine brain likes consistency
Do all you can to eat at consistent times and keep nonperishable snack items with you for those times that you cannot get a proper meal. Being prone to migraine often means you must be more vigilant about keeping a routine to keep your brain happy.
Some people find that they can reduce their migraine frequency by making sure they have at least a small snack every few hours. Others avoid sleeping late when they do not have morning commitments so that their mealtime is consistent.
Morning headaches after sleeping late may also be due to delayed caffeine for those who are accustomed to having caffeine each morning.
2. Sugar is an inflammatory food
I think the overwhelming majority of people agree that adding sugar is not a healthy practice. Over the past few years, as certain chronic, inflammatory diseases have risen along with the steep increase in our sugar consumption, more research is being done linking sugars and simple carbohydrates to preventable diseases.
Just having daily sugary drinks can increase biochemical markers of inflammation in healthy people. Additionally, diets high is refined sugars and starches may also lead to increased illnesses associated with inflammation.
How is this relevant to migraine? Increasingly, experts believe that chronic inflammation plays a role in migraine. Perhaps the sugar and migraine connection has to do with neurogenic inflammation that can be influenced by several factors including what we eat.
What about anti-inflammatory diets?
While there is no one anti-inflammatory diet that nutrition professionals can agree upon, all the diet approaches to reducing inflammation significantly limit sugars and refined carbohydrates. The Mediterranean diet is a popular approach to reducing inflammation in the body. Healthline has a good overview of the Mediterranean diet and specifies avoiding “added sugar, soda, candies, ice cream, table sugar and many others.”
During the 2022 Migraine World Summit, one of the experts discussed the topic of migraine and obesity. His recommendation was to consider the Mediterranean diet as a healthy approach to weight management and overall wellness.
It is my opinion that there are some people who have no food triggers. However, they may be helped by avoiding their inflammatory foods. I consider a diet high in sugar and highly processed foods to be inflammatory.
The ketogenic diet is another approach to managing migraine through diet. If you can see a clear relationship between sugar and migraine attacks in your life, ask your doctor for a referral to a registered dietitian to get you started on a well-formulated plan. A low-carb diet rather than one that produces consistent ketones may be enough to bring about some relief.
3. Other common migraine triggers in sugary foods
Sometimes people may erroneously assume the triggering factor in their food choice was sugar. When it was actually something else in the sweet treat. Sugary foods are often combined with other ingredients that are considered common migraine triggers such as nuts, chocolate, food colorings and certain dried fruits.

Determining migraine foods triggers can be very tricky especially when you have frequent attacks. From observation, some people have a handful of common foods that are triggering. So, eliminating one food at a time often does not yield results. For example, they may avoid yogurt while continuing the eat nuts and protein bars (common migraine triggers) while being sensitive to all three foods. It can be quite frustrating especially since many well-meaning “experts” suggest avoiding suspected foods one at a time.
For people with high-frequency episodic migraine and chronic migraine, committing to the Heal Your Headache plan developed by Dr. David Buchholz or the Charleston Diet by Dr. Carol Foster is often an effective approach to figuring out food triggers. The Charleston Diet is designed to avoid the common migraine trigger foods while stabilizing blood sugar levels. Dr. Foster spends a lot of time discussing how to pair foods to minimize wide fluctuations in blood sugar. I was terribly frustrated while trying to figure out my food triggers until I did a full elimination diet. It was incredibly helpful for me and many others with migraine.
A note about chocolate
There are countless social media memes and quotes about this unique, celebrated simple pleasure in life. At Migraine Strong we are committed to people living their best lives… and that often includes chocolate. Please do not assume chocolate is one of your personal food triggers because you’ve heard others mention it and it’s “on a list.” This is an excellent article about chocolate and migraine and a must-read if you’ve been avoiding it or are thinking of avoiding it.
4. When headache from eating too much sugar is really prodrome, the first phase of migraine
What if the migraine attack was already set in motion before the sweet tooth was satisfied? What if there is truly no relationship between sugar and migraine for you?
Migraine has 4 distinct phases and understanding them helps to minimize the frequency and intensity of attacks.
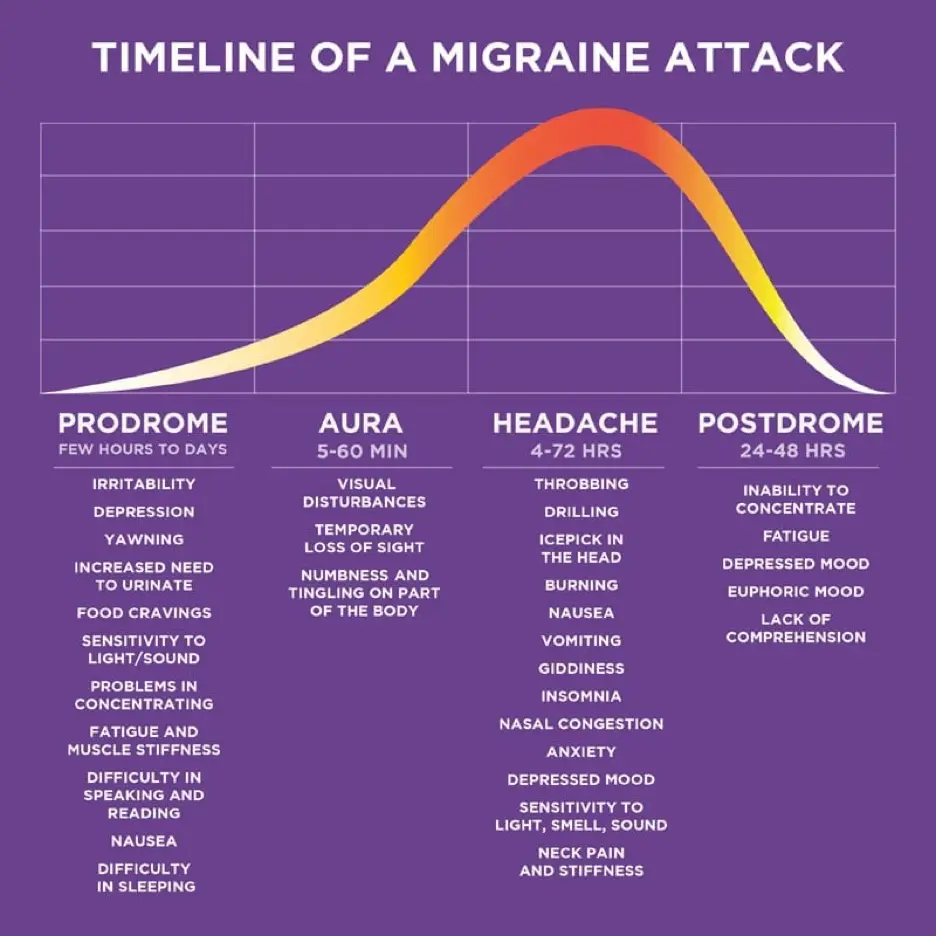
In the first phase, prodrome, many people experience intense food cravings. For some people, prodrome has them reaching for salty foods like potato or corn chips. For others it is probably best to not get between them and the Haagen Dazs ice cream or bag of gummy bears. BUT, prodrome is shortly followed by aura (for some) and the full attack phase of migraine. So, while there may be a notable pattern: sugar craving +overdoing it with sweets= migraine, the sugar may not be to blame. The attack was going to happen with or without the goodies… and darn! Those Oreos were good!
Information is key regarding sugar and migraine
As with most aspects of getting migraine attacks under good control, it starts with educating yourself about the complexities of migraine and the human body. Then comes determining a strategy to find the right combination of interventions that work best. Diet is a great preventive strategy to try along with other aspects of the Treatment Pie.
As a registered dietitian passionate about helping people with migraine, I suggest limiting sugars and highly processed foods. This is good for overall wellness, attaining and maintaining a healthy weight and helping to reduce the burden of migraine.
If you need help figuring out which migraine diet approach may be best for you, this blog a must-read. There is no one “migraine diet.”
This article has been updated and refreshed from the original publication in March, 2021.



It took me forever to realize my migraines were due to reactive hypoglycemia. None of my doctors suggested it or figured it out, and when I brought it up once they even said they had no idea and I should talk to my GP. Sadly, we often have to do a lot of this work on our own!